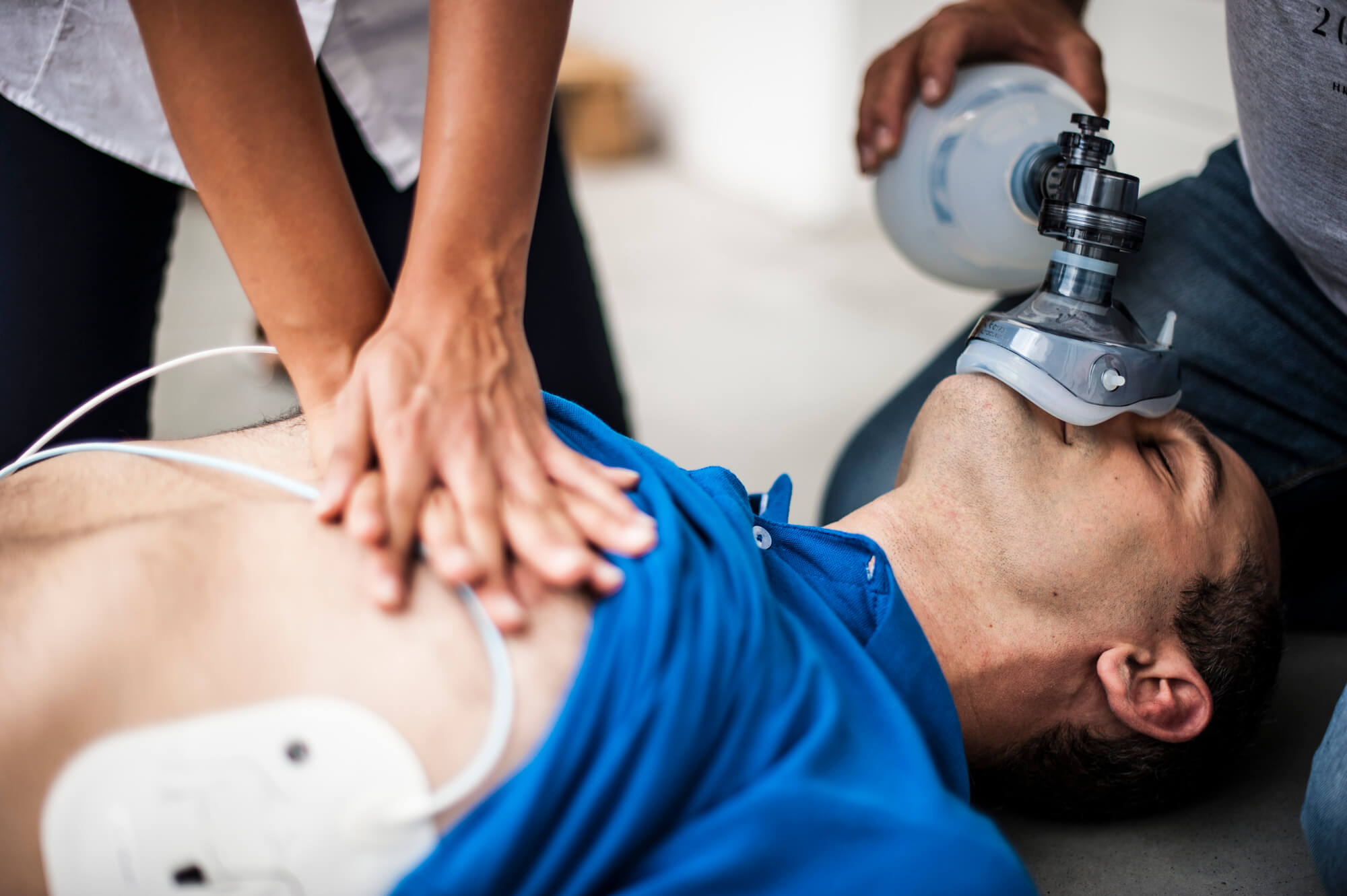
Treat and care for your cardiac arrest patients using the proper techniques and approach. Read more to find out the steps today:
Time is crucial when it comes to treating a patient in cardiac arrest. As a nurse or doctor, you need to be able to quickly assess the threats to your patient’s survival, identify which ones to address first, and then take the appropriate actions.
The ABCDE approach makes it easy to remember how to evaluate a patient in cardiac arrest, and it works well for many trauma patients also. This standardized treatment model also helps medical personnel work together because they don’t waste valuable time discussing the next step to take - everyone is on the same page. If you’re studying to be a doctor or nurse, it’s crucial to memorize the ABCDE approach to assessing and treating cardiac arrest patients.
Table of Contents:
Airway
Generally practiced as the first step for a very good reason, ensuring the victim does not have a life-threatening obstruction in their airways is important to not losing your patient in the first few vital minutes that you have. Even in cases where the patient survives, airway obstruction can cause damage to the kidneys, heart, and brain. An obstructed airway should always be treated as an emergency. Here are the key steps to take:
- Determine whether the airway is obstructed (partially or completely): Listening to the patient’s voice is the first step.
- If they can speak normally, the airway is patent.
- A partially obstructed airway will cause the voice to sound abnormal, and breathing will be noisy. The sound of snoring is an example of a partially obstructed airway.
- A fully obstructed airway can be indicated by “see-saw respirations” of the chest and abdominal muscles and/or a lack of breath sounds despite the patient’s efforts to breathe.
- Attempt to open the airway: If no equipment is available, you can use the head-tilt and chin-lift maneuver to open the airway. If equipment is available, use it to remove the obstruction via suction.
- Follow current guidelines to treat completely airway obstruction: If the patient is conscious, use alternative back blows and abdominal thrusts (five of each before alternating) to clear the obstruction. With an unconscious patient, you should initiate CPR after calling for help.
After the airway is opened, it’s essential to provide the patient with high-concentration oxygen as soon as possible.
Breathing
Diagnosing and assessing the respiratory rates is vital to diagnosing and treating immediately life-threatening conditions such as acute/severe asthma, pulmonary edema, tension pneumothorax, and more. The goal is to assess whether the patient’s breathing is sufficient, and to treat the cause if it is not.
- Monitor the patient for signs of respiratory distress: Abdominal breathing, sweating, use of auxiliary respiratory muscles, distended neck veins, and/or cyanosis.
- Determine the respiratory rate: Between 12 and 20 breaths per minute is normal. A high respiratory rate may indicate a problem.
- Observe the depth of each breath:onitor the respiration rhythm and note whether the chest expands equally on both sides.
- If possible, apply a pulse oximeter: Record the patient’s oxygen concentration.
- Listen for abnormal breathing sounds: Wheezing, inability to take a deep breath or cough, rattling noises).
- Percuss the chest: Determine if there is dullness (possible pleural fluid) or resonance (possible pneumothorax).
- If a stethoscope is available, auscultate the chest: Determine if the patient is experiencing lung consolidation, pleural fluid, and/or pneumothorax.
The exact cause of the respiratory issue will determine the correct treatment. It’s always important to provide oxygen to patients who are in a critical state. If the patient is experiencing insufficient breathing, you may assist using rescue breaths or a bag-mask if one is available.
Circulation
We recommend always considering hypovolaemia to be the primary cause of shock until proven otherwise. It’s also essential to remember that breathing problems (which should be dealt with before circulation) can affect a patient’s circulatory state. Here are some steps for assessing circulation:
- Assess the skin color: Check the hands and fingers for a blue, pink, or mottled appearance.
- Look for sweating and/or a hot or cool limb temperature: This can indicate a circulation issue.
- Determine the pulse rate: Use a stethoscope to listen to the heart, if possible.
- Calculate the capillary refill time (CRT): Use pressure on a fingertip to cause blanching and then count how long it takes the skin to return to the same color as the surrounding skin. A normal CRT is less than 2 seconds, but outside factors (such as a cold room) can affect the time.
- Take the patient’s blood pressure: Do this as soon as possible.
- Look for other signs of circulation problems: Check for a decreased level of consciousness or external or concealed bleeding.
You can give fluid intravenously to patients who are experiencing a fast heart rate and cool peripheries as long as there are no clear signs of cardiac arrest. If the patient starts to exhibit signs of cardiac failure, decrease or stop fluids. Patients who are experiencing chest pain and showing signs of a possible acute coronary syndrome (ACS) should be treated accordingly with oxygen, aspirin, nitroglycerine, or other common treatments.
Disability
Diagnosing disabilities usually begins with asking yourself if the patient has any life-threatening disabilities such as hypoxia, hypercapnia, and cerebral hypoperfusion, which are common causes of unconsciousness. Here are some steps to determine the level of consciousness:
- Use the AVPU method to grade the patient on their (A) alertness, (V) voice responsiveness, (P) pain responsiveness, or (U) unresponsiveness. The Glasgow Coma Scale is an alternative assessment method.
- Review steps A, B, and C, to exclude or treat hypoxia and hypotension.
- Examine how the pupils appear and react to light.
- Monitor the patient’s limb movements to evaluate lateralization.
- Measure the patient’s blood glucose level; low blood glucose can cause a decreased level of consciousness but can be treated quickly with infused or oral glucose.
If possible, determine whether any sedatives or analgesic drugs have been recently administered and provide treatment when possible. Make sure to keep an unconscious patient in a lateral position to protect their airway.
Exposure
To diagnose your patients properly, full exposure of the body is usually necessary. We recommend always respecting your patient’s dignity and minimizing heat loss as much as possible when removing clothing to assess the patient’s condition further.
During a full physical examination, you should look for any clues to help you determine the cause of the patient’s condition. Some examples are needle marks, bleeding, rashes and other skin reactions, abnormal body temperature, and signs of trauma. Use any information you gain to guide ongoing diagnosis and treatment.
Treat Your Cardiac Arrest Patients Effectively With the ABCDE Approach
As a nurse or doctor, you need to know how to react to a patient in cardiac arrest. The ABCDE approach is easy to remember and can help you follow the correct steps to potentially save your patient’s life: airway, breathing, circulation, disability, and exposure. Following these steps ensures that you identify and address the most crucial issues first.
These steps, as well as other essential actions, are all part of our Advanced Cardiac Life Support Certification (ACLS) program. With our ACLS course, you can certify or recertify to ensure you have the knowledge and skills required to help cardiac arrest patients. Maintaining your ACLS certification ensures you have the skills you need to give your patients the best care. With up-to-date credentials, you’re ready to respond to career opportunities when they arise.
At eMedCert, we know that doctors and nurses have busy schedules. That’s why our ACLS Certification program is completely online. We also offer Basic Life Support (BLS) and Pediatric Advanced Life Support (PALS) Certification and Recertification programs online. Study the material at your own pace and take the exam whenever you feel ready. If you don’t pass the first time, you can take the test again as many times as you want. With our certification and recertification bundles, you can get all the essential credentials you need for an affordable price.